
COVID-19 Pandemic: How to protect yourself and the others
Posting Date: 3/30/2020Author: Huagui Li, MD, PhD *
* About the author: Dr. Huagui Li is a licensed cardiologist at M Health Fairview. He is a lifetime member of the Association of Minnesota Chinese Physicians (AMCP), former president, and currently the Education Program Director. He chairs the medical advisory subcommittee of AMCP COVID-19 relief fundraising task force.
COVID-19 is a virus disease that is transmitted by 3 possible routes: contact, droplet and airborne. The virus invades the human body mainly through the mucus membrane of the respiratory tract, and possibly the eyes.
How to prevent the contact transmission? Contact transmission is probably the most common route. Prevention of the contact transmission is extremely difficult. Since the virus is known to survive up to 3 days on certain surfaces (plastic and stainless steel), viable virus could be present on the surfaces of different objects. Any surface or object in the public and work places could be virus-contaminated by the body fluid or virus-laden hand of an infected person. During the current epidemic with the possible presence of asymptomatic virus carriers, the risk of touching a virus-contaminated surface is real. In places like stores, airports or on the buses, trains or airplane, the opportunities of touching a virus-contaminated object could be too many. Hand hygiene cannot be over emphasized but may not be easily implemented. Not touching your face without washing or treating your hands with a sanitizer may be nearly impossible to do but you must do it. In addition, you must avoid contaminating your clothing, credit cards, purse or wallet, cell phone, keys and steering wheel of the car. If you pay close attention to every step by using good hand hygiene, your probability of getting infected will be significantly reduced. This is one of the rationales for "shelter in place" because to stay at home is the safest.
However, health care workers cannot "shelter in place". For health care workers, the risk of contact transmission in the health care facilities may be higher than public places because of the presence of infected patients. To open a door, to move a chair, to use the computer keyboard or mouse could subsequently transmit the virus to your body parts or clothing if one of the objects is virus-contaminated. If you accidentally touch the outside of a contaminated mask without washing hands, you may end up with infection, regardless how great the mask is. In particular, when you enter the room of an infected patient with all the fancy protection gears, you can get contaminated accidentally if you make a mistake during the removal of the protection gears. A contaminated stethoscope in the room of an isolated patient can serve as transmission tool if it is not treated properly before use.
How to prevent the droplet transmission? Most of us know that droplets are produced when a person coughs or sneezes. However, few of us know that droplets can also be produced when a person speaks, although not as much as coughing or sneezing. Fortunately, the droplets contain water and fall to the ground or floor within 10 minutes. Most of the heavy droplets travel only about 1 meter. The social distance of 6 feet (about 2 meters) is set arbitrarily but will significantly reduce the risk of droplet exposure from each other. It has been reported that the droplets from coughing or sneezing can travel up to 200 feet (about 60 meters). In addition to social distancing, wearing a mask helps to reduce the risk of droplet exposure.

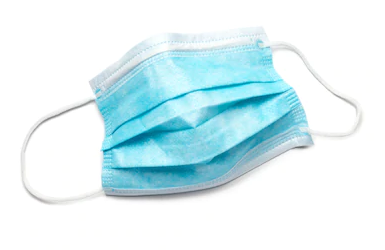
Surgical mask: It is easily available and has a low cost. It is more comfortable than N95 and less likely to get wet from your own breathing. It has 3 layers and is designed to block particles (including droplets) sized >10 µm in diameter, with >95% filter efficiency. The surgical mask prevents the wearer’s own droplets from going out into the air to contaminate the others. At the same time, it prevents the droplets from the others to get onto your nose and mouth. The surgical mask cannot prevent aerosol-sized particles (<10 µm) from getting into your respiratory system because the aerosol-sized particles are small enough to pass through the filters of the surgical mask during breathing. The aerosol particles can also easily pass through the unsealed mask-face interface.

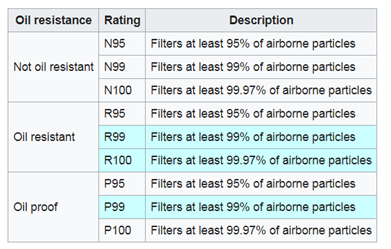
How to prevent airborne transmission? I use the term airborne to define transmission that is caused by virus-laden aerosol. Aerosol-sized particles are <10 µm. Unlike droplets which fall to the ground within 10 minutes, aerosol particles can suspend in the air for long time. The coronavirus is spherical and has a diameter of 0.06-0.2 µm which is much smaller than the filtering size of 0.3 µm for N95. However, the virus itself is unlikely free floating in the air and is probably attached to other larger particles. The scientists from US CDC have found that SARS2-CoV19 virus can survive up to 3 days on certain surfaces and more than 8 hours in the air. It is generally believed that only certain medical procedures such as endotracheal intubation in the hospital environment can produce aerosol. However, some experts have argued that any infected person can generate virus-containing particles within the range of aerosol size. Theoretically, after evaporation of water, a virus containing droplet can release the virus into the air to produce virus-laden aerosol if the floor or any surface is disturbed by human traffic or natural air flow. Indeed, respiratory viruses have been detected in the air of the enclosed space on the train of the Singapore city railway system, although the detected virus was probably not viable or infectious. Thus, airborne transmission is possible in the enclosed space if there is an infected person but the probability is uncertain. We must realize that the coronavirus may still be able to penetrate a tightly fit N95 mask through diffusion from the capillary effect if the mask gets wet and is worn for a long time.
To my knowledge, there is no evidence of virus-laden aerosol in the outdoor air. Thus, I can understand why the US government does not restrict outdoor activities. The value of wearing a mask in the outdoor environment is unknown. The risk of getting infection from outdoor activities is probably near zero as long as you do not get close to the other people or touch any object. Overall, it is not possible or feasible to prevent airborne transmission for the lay public but fortunately such a risk is extremely low for them. The best protection is to follow the shelter in place policy and stay at home.
To prevent airborne transmission in the hospital environment, the airborne precaution protocol is applied to any patient with suspected or confirmed diagnosis of COVID-19 at the present time. This protocol involves placing the patient in a negative pressure room so that the patient’s room air does not get to the other indoor space of the hospital. Staff taking care of the patient may wear airborne protective gears including tight-fit N95 plus eye protection goggles or even better protective devices. Most importantly, every staff must get trained on how to put on and remove the protective gears properly without contamination. In addition, our hospital has designated monitoring staff to watch for any accidental breach of the protocol.
